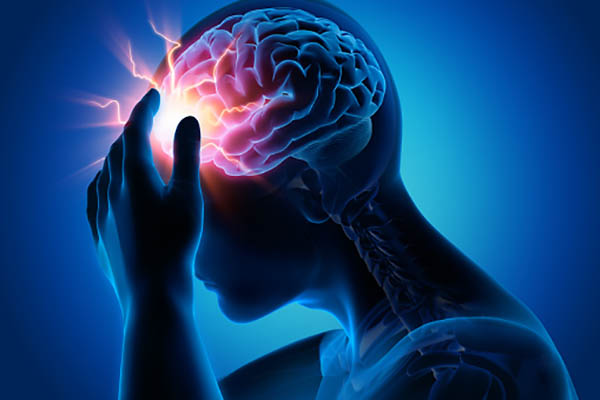
A throbbing, pounding headache, bright zigzagging lines across your field of vision, sensitivity to light lingering fatigue, disrupted sleep. A migraine can include any of these symptoms. while an incapacitating headache is one of the most common experiences of migraine.
To trace a migraines anatomy, we have to begin in the days and hours leading up-to migraine. When people often identify warning signs ranging from a fatigue or mood changes to bursts of yawning, sleep disruption, nausea, lights and sounds sensitivity and even increased thrust these warning sighs point to a peculiarity part of the brain hypothalamus. The hypothalamus normally controls the system behind these symptoms our bodies internal hormonal balances, circadian rhythms and water regulation. It had wide connections throughout the brain and is more active than usual in the days before migraine.
Another common warning sign is the migraine aura, which can take the form of transient visual changes, tingling or even trouble speaking. These sensations come from a change in charge across cell membranes that leads to spreading changes in brain activity and blood flow.
During the headache phase the trigeminal nerve place a key roll. This nerve normally transmits touch, temperature and other sensations from the skin to the most of the face, part of the scalp and some of the blood vessels and layers covering the cerebral cortex. Once activated this nerve transmits pain signals.
During a migraine this pain pathway becomes sensitized meaning the threshold for provoking pain is lowered. Sensations that would usually be pain free such as coughing, bending over or light and sound can become pain full.
Migraines are as common as they are diverse, effecting as many as 33% of women and 13% of men in their life times. Migraines is a neurological disorder effecting multiple parts of the brain the brain-stem, cerebral hemispheres and nerves themselves. Hormonal fluctuations are thought to have a roll in some of these things some women experience the significant reduction in migraine frequency. After menopause, when sex Harmon fluctuations are fewer. Meanwhile just before menopause these fluctuation increase and some women experience worsening or new headaches.
People with migraines are more likely to suffer from depression, panic disorder, sleep disorders and strokes. The relationship with these diseases is likely complex, possibly reflecting the effect of migraine on those diseases or vise versa or reflecting their shared genetic basis.
Also Read – Your Sleeping Position Reveals These Personality Traits